Sharon has 21+ years of experience as a qualified Emergency Care Nurse registered with the Australian Health Practitioner Regulation Agency (APHRA) and 12+ years as a First Aid Trainer.
She takes pride in FirstAidPro making first aid training available, comprehensive and affordable to everybody.
A dog bite is an injury caused when a dog’s teeth break the skin, creating a puncture, laceration, abrasion or crush injury that can lead to infection, tissue damage and other medical complications. This article explains the essential first aid steps, symptoms to watch for, how to prevent infection, when to seek medical attention, and what every Australian needs to know about dog attacks, tetanus, rabies, animal and human bites, and possible complications.
Want to feel confident responding to a dog bite, animal bite or human bite? Enrol in a nationally recognised first aid course with First Aid Pro today.

Key Takeaways: Dog Bite – Symptoms, Risks & First Aid
- Any dog bite where the skin is broken carries a high risk of infection, especially puncture wounds and bites to the hand or face.
- Wash the wound immediately with soap and water, apply a sterile bandage, and monitor closely for swelling, redness, or increasing pain.
- Seek medical attention for deep wounds, bites from unfamiliar dogs, signs of infection, or if the bite involves a child, joint, tendon, or face.
- A tetanus booster may be needed if your vaccination is out of date or the wound is deep or contaminated.
- While rabies is not present in Australian dogs, Australian bat lyssavirus and overseas bites may require urgent rabies vaccination.
- Dog, cat and human bites all have different bite injury patterns but share a significant risk of bacterial infection and should be treated seriously.
- Proper first aid, early medical review, and safe interactions with dogs all help reduce the risk of long-term complications.

Understanding Dog Bites and Why They’re a Serious Medical Concern
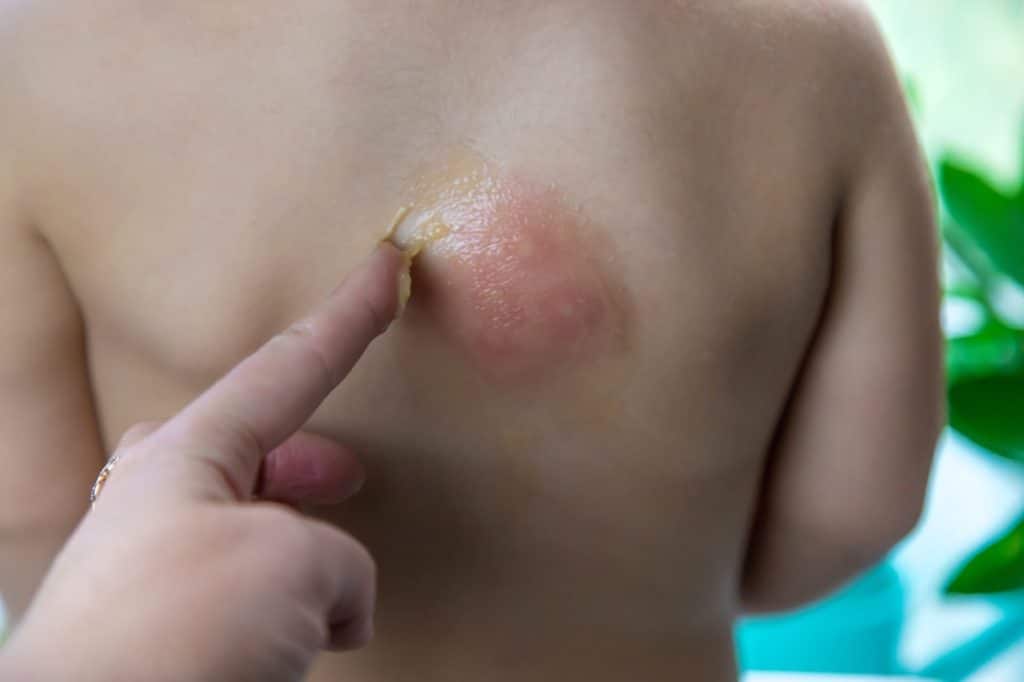
Dog bites are common injuries in Australia, often caused by pets, excited dogs, frightened animals, or misunderstandings during play. While many bites appear minor, any time the skin is broken, there is a high risk of infection due to bacteria found in a dog’s mouth, on human skin and in the environment.
Dog bite wounds typically involve:
- Puncture wounds – can penetrate deeply and hide extensive tissue damage.
- Lacerations – tearing, ripping or slicing injuries.
- Crush injuries – common in bites to the hand or foot.
- Abrasion injuries – scraped or grazed skin.
These injuries may affect tendons, nerves, muscles, blood vessels, or bones. A dog bite can cause rapid-onset infection within 24 hours, especially in hand or finger wounds, which are particularly vulnerable.
Types of Bites: Dog Bite, Cat Bite, Human Bite and Other Animal Bites

Animal and human bites share many similarities, including a high chance of bacterial infection. Cat bites penetrate deeply, while human bite wounds carry some of the highest bacterial loads of all bite injuries. Understanding the differences helps you administer first aid correctly.
Comparison Table: Dog, Cat and Human Bites
Bite Type | Common Injury Patterns | Risk of Infection | Typical Bacteria | Notes |
Dog bite | Puncture, crush, ripping, tearing | Moderate–high | Pasteurella, Staph, Strep | Can cause tendon or joint damage |
Cat bite | Deep puncture wounds | Very high | Pasteurella multocida | Infection can start within hours |
Human bite | Laceration, crush, bruising | Very high | Eikenella, Strep, Staph | Considered a contaminated wound |
Other animal bites | Varies | Moderate–high | Varied bacteria | Depends on species |
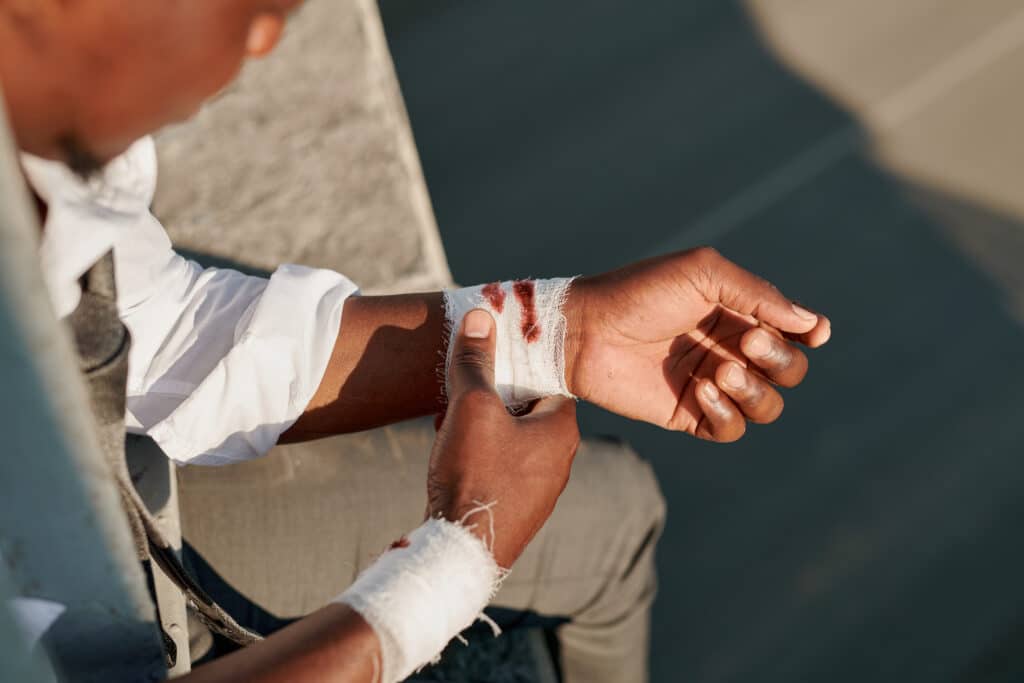
Immediate First Aid for Dog Bites: A Step-by-Step Guide
If you’ve been bitten by an animal, especially a dog, fast and accurate first aid helps reduce the risk of infection and possible complications.
Stop Heavy Bleeding and Get Safe
If bleeding is heavy or spurting, apply firm, direct pressure with a clean cloth and seek emergency care immediately. Once you are safe from the dog and major bleeding is controlled, continue with wound cleaning.
Wash the Wound as Soon as Possible
Use soap and water, and let cool running water flow over the bite wound for several minutes to help remove dirt, saliva and bacteria. Do not scrub vigorously, as this may damage tissue.
Apply Antiseptic and Cover the Wound
If available, apply an antiseptic or antibacterial cream or ointment after washing. Use a sterile bandage, gauze pad, or clean dressing to cover the area, and do not tape tightly, as restricted circulation increases the risk of complications.
Avoid Aggressive Squeezing
Do not aggressively squeeze, poke or “milk” the wound, as this may force bacteria deeper into the tissue. A little natural bleeding is acceptable, but avoid deep or forceful pressure on the wound edges.
Step 5 — Seek Medical Advice
You should see a doctor or seek immediate medical attention if:
- the wound is deep, a puncture, or of uncertain depth; you were bitten by an unfamiliar or unvaccinated dog;
- the wound is on your hand, foot, face or near a joint;
- you develop signs of infection such as redness, warmth, swelling, pus or fever;
- you have a chronic condition (such as diabetes, immune suppression or poor circulation) that increases infection risk;
- or you have not had a tetanus vaccination in the past five years, especially if the wound is deep or dirty.
In areas where rabies is a concern, seek urgent medical advice after any bite from an unfamiliar, sick, or strangely behaving dog, as you may need rabies post-exposure treatment.
➡️ Protect yourself and others by learning proper bite treatment and first aid skills. Enrol in a First Aid Pro course today.
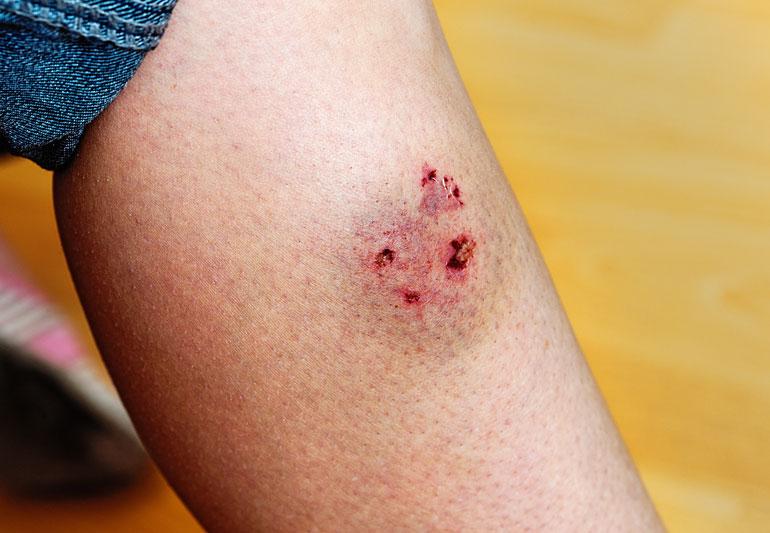
Signs of Infection: What to Look For Within 24 Hours
A dog bite can cause infection even if it appears minor at first. Because puncture wounds penetrate deeply, the wound appears small but hides serious internal damage.
Recognising Infection After a Dog Bite
Early Signs of Infection
- Increasing pain
- Redness and warmth
- Swelling
- Pus or discharge
- Fever
- Red streaks leading from the wound
Late or Severe Infection Signs
- Rapid swelling of fingers or hands
- Loss of movement
- Difficulty bending or extending joints
- Severe fever
- Signs of sepsis
Important: If any of these symptoms occur, you need immediate medical attention at an emergency department.
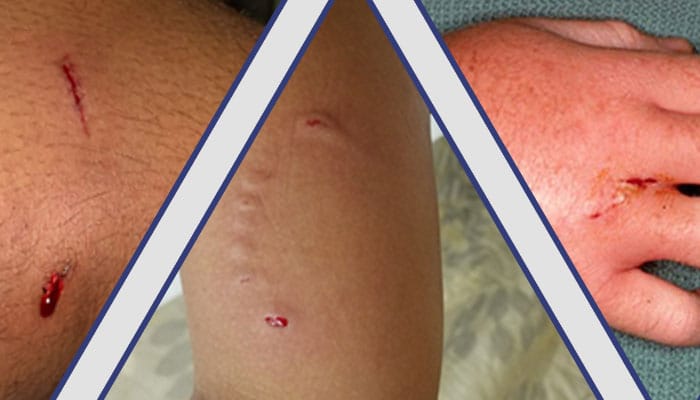
Dog Bite Bacteria and Why Infection Spreads Quickly
Dog bite infections are commonly caused by several types of bacteria. These germs can penetrate deeply into bite wounds and spread rapidly if not treated.
Common Dog Bite Bacterium
Pasteurella
Pasteurella is frequently found in dog bite wounds and often causes rapid swelling, pain and tenderness around the bite within hours of injury.
Skin and Soft-Tissue Infections
Staphylococcus aureus
Staphylococcus aureus can lead to painful, pus-filled infections, especially when the skin barrier is broken by a bite and bacteria enter deeper tissues.
Spreading Redness and Pain
Streptococcus species
Streptococcus species are linked with cellulitis, where redness, warmth and pain spread out from the bite site along the skin and lymph vessels.
High-Risk Complications
Capnocytophaga canimorsus
Capnocytophaga canimorsus can cause life-threatening illness in vulnerable people, including those with diabetes, liver disease or weakened immune systems.
Tetanus and Dog Bites: Do You Need a Vaccination?
Dog bites are considered tetanus-prone wounds. If the skin is broken, tetanus bacteria may enter via dirt or saliva.
You may need a tetanus booster if:
- Your last shot was more than 5 years ago
- The wound is deep or contaminated
- You are unsure of your vaccination status
Tetanus in Australia
Tetanus cases are rare due to vaccination, but bite injuries remain a major trigger for the cases that do occur.
Rabies, Australian Bat Lyssavirus and Animal Bites
Although terrestrial rabies is not found in Australian dogs, Australian bat lyssavirus (ABLV) is present in some bat populations and can cause a rabies-like illness in humans.
Understanding the Risk
Any bat bite or scratch must be treated as potentially serious. ABLV is rare but can be fatal if not managed with prompt post-exposure treatment.
- Found in some Australian bat populations
- Causes a disease similar to rabies
- Can be prevented with urgent vaccination after exposure
If You Are Bitten or Scratched by a Bat
- Wash the area with soap and water
- Seek immediate medical attention
- You may need a rabies vaccine course
Travel reminder: International travellers bitten by an animal overseas may also need post-exposure rabies vaccination. Always seek urgent medical advice after any bite from a bat or unknown animal.
How to Clean and Bandage Dog Bite Wounds Correctly
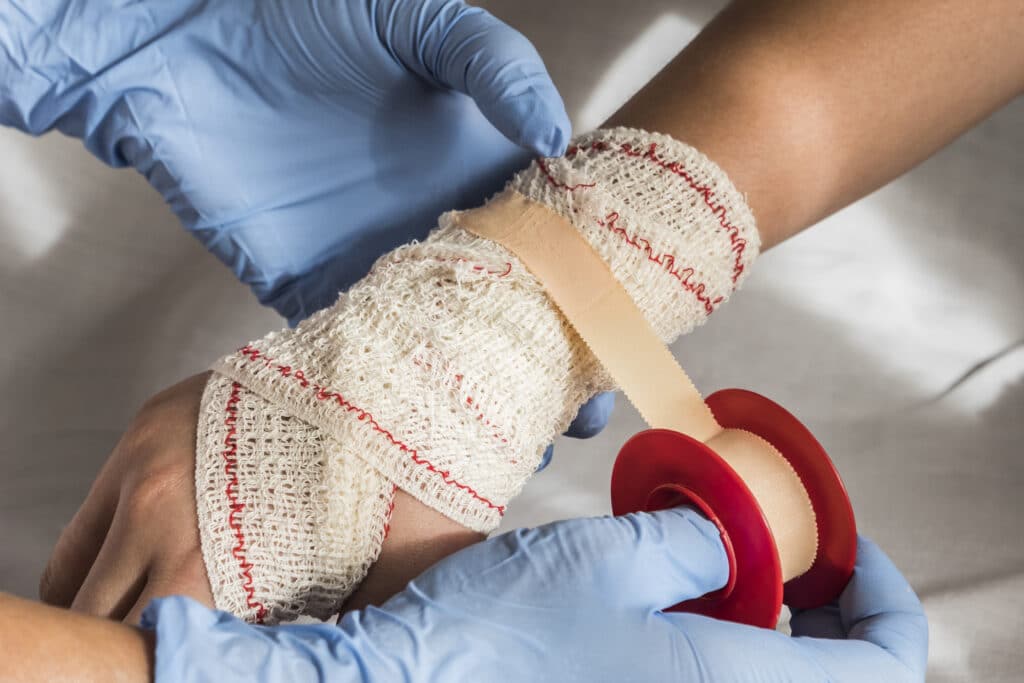
Proper wound care reduces the risk of infection.
First Aid Cleaning and Bandaging Steps
Step | Action | Why It Matters |
1 | Wash with soap and water | Removes bacteria |
2 | Let water run over wound | Flushes contaminants |
3 | Pat dry with clean cloth | Prevents irritation |
4 | Apply sterile bandage | Protects broken skin |
5 | Change bandage daily | Reduces bacteria growth |
When You Need Medical Attention After a Dog Bite
Some dog bite injuries require urgent assessment. Recognising when to seek medical care helps prevent serious infection, tendon damage and other complications.
Seek Medical Care Immediately If
- The bite is a deep puncture
- You cannot fully move a finger, hand or limb
- The wound is on the face
- You suspect bone or joint involvement
- The wound appears infected
- You experience fever or chills
- A child was bitten
- You were bitten by a dog not known to you
What Doctors May Do
- Clean and debride the wound
- Prescribe antibiotics
- Assess tendon or nerve damage
- Provide a tetanus booster
- Order X-rays if bone injury is suspected
Important: Do not wait to see if a serious bite improves on its own. Early treatment in an emergency department or medical clinic can reduce the risk of long-term problems.
Possible Complications of Dog Bite Wounds
Untreated dog bite injuries can lead to serious complications that affect skin, soft tissue, nerves, tendons and even bone. Early first aid and medical review help reduce these risks.
Infection and Tissue Damage
- Cellulitis
- Bone or joint infections
- Blood poisoning (sepsis)
Movement and Function Problems
- Tendon injuries
- Scarring or nerve damage
- Loss of function in fingers or hand
Important: Some injuries require surgical care to repair damaged tissue and restore movement. Do not ignore bite wounds that are deep, painful or getting worse.

Cat Bites, Human Bites and Other Animal Bites: When They Require Immediate Medical Attention
Cat bite wounds are notorious for causing rapid infections due to deep punctures.
Human bite wounds carry extremely high bacterial loads and should always be assessed by a healthcare professional.
If you’ve been bitten by an animal or human, especially on the hand, face or near a joint, you may need immediate medical attention to prevent long-term complications.
Knowledge Test: Dog Bite First Aid Quiz
Test your understanding of dog bite first aid. Tap or click an answer for each question to see if you’re correct, then use the reset button to try again.
1. What is the first thing you should do after a dog bite?
2. When should you seek medical attention?
3. What is a major risk from deep puncture wounds?
4. Which disease may require vaccination after a bite?
5. When is rabies vaccination needed?
➡️Take your knowledge further — Enrol in a nationally recognised First Aid Pro course and learn to administer first aid confidently and correctly.
References
- HealthDirect Australia – Dog bites and first aid
- Royal Children’s Hospital Melbourne – Animal & Human Bites
- Better Health Victoria – Bites and Stings
- Queensland Health – Rabies and ABLV
- Australian Immunisation Handbook – Tetanus recommendations
Frequently Asked Questions
If the skin is broken, the wound is deep, or infection signs appear, you should seek medical care. Hand and foot bites always require assessment.
Wash with soap and water, apply a sterile bandage, and monitor closely. See a doctor if swelling or redness increases.
You may need a tetanus booster if your vaccination is out of date or the wound is deep.
Yes. Tendon, nerve or bone injuries are possible, especially from puncture wounds.
Dog-related rabies is not present in Australia, but bat bites may transmit Australian bat lyssavirus. Overseas bites may require rabies vaccination